Gwyneth Paltrow Opens Up About Her Menopause Experience
Gwyneth Paltrow Opens Up About Her Menopause Experience
Gwyneth Paltrow Opens Up About Her Menopause Experience
A study1 published at the National Library of Medicine focused on the effects of two natural herbs, black cohosh and St. John’s wort, on symptoms commonly experienced by women during menopause, often referred to as climacteric symptoms. These symptoms can include hot flashes, mood swings, and other physical and emotional changes. Traditionally, women have turned to hormone therapy to manage these symptoms. However, concerns about potential side effects, like an increased risk of breast cancer, have led many to seek natural alternatives.
In this research, 89 women going through menopause were divided into two groups. One group was given a combination of black cohosh and St. John’s wort, while the other received a placebo, which is essentially a sugar pill with no therapeutic effect. The study lasted for 12 weeks, and the women’s symptoms were regularly assessed using a standard measure called the Kupperman Index.
The results were promising. Women who took the herbal combination reported a significant reduction in their menopausal symptoms, especially hot flashes, compared to those on the placebo. Additionally, there was an interesting observation related to cholesterol. The “good” cholesterol (HDL) levels in the herb-taking group slightly increased, which is a positive sign for heart health.
In simple terms, the combination of black cohosh and St. John’s wort seems to offer relief from menopausal symptoms and might even have a beneficial effect on cholesterol levels. This suggests that these herbs could be a natural alternative for women seeking relief from menopausal symptoms without resorting to traditional hormone therapy. However, as with all treatments, it’s essential to consult with a healthcare professional before making any decisions.
This study offers valuable insights for women and their families, especially those going through menopause and experiencing its associated symptoms:
For women (and their families) navigating the challenges of menopause, this study offers hope for a natural, potentially safer way to manage their symptoms and improve their overall well-being. However, it’s always crucial for individuals to consult with healthcare professionals before starting any new treatment or therapy.
1Chung DJ, Kim HY, Park KH, Jeong KA, Lee SK, Lee YI, Hur SE, Cho MS, Lee BS, Bai SW, Kim CM, Cho SH, Hwang JY, Park JH. Black cohosh and St. John’s wort (GYNO-Plus) for climacteric symptoms. Yonsei Med J. 2007 Apr 30;48(2):289-94. doi: 10.3349/ymj.2007.48.2.289. PMID: 17461529; PMCID: PMC2628120. | Copyright © 2007 The Yonsei University College of Medicine
Sarah Stern began experiencing sudden hot flashes, irregular menstrual cycles, sleep disturbances, and night sweats in her early 30s. Initially confused, she later learned from a fertility clinic that she was in perimenopause. Perimenopause is a transitional stage leading up to menopause, which can begin a decade before menopause. While menopause technically lasts only one day (marked by 12 months without a period), perimenopause can cause various symptoms. Many women, like Sarah, feel that the medical community doesn’t adequately recognize or address perimenopause symptoms.
What Is Perimenopause? Perimenopause is the period immediately before menopause. It typically occurs during a woman’s 40s, but some might notice changes as early as their mid-30s. During this phase, women may observe subtle alterations in their menstrual cycle length, duration, and flow. This is also when fertility starts to decline due to fluctuating hormone patterns. On average, perimenopause lasts for four years, but it can be as short as a few months. In the final one or two years leading up to menopause, the drop in estrogen becomes more pronounced, leading to menopausal symptoms even while menstruating. A good predictor of when perimenopause will start is the age at which one’s mother entered menopause.
Symptoms of perimenopause include changes in menstrual cycles, mood shifts, hot flashes, sleep disturbances, and more. While there’s no specific test to diagnose perimenopause, tracking symptoms can help. Treatments for symptoms range from oral contraceptives to hormone therapy and even some antidepressants. Non-hormonal treatments, such as cognitive behavioral therapy and hypnosis, have also been found effective for hot flashes.
It’s essential for women to educate themselves about perimenopause, monitor their health, practice self-care, and find a supportive community to navigate this life transition.
Stages Leading Up To Menopause:
First Sign Of Perimenopause: The initial sign of perimenopause is typically a disruption in the menstrual cycle. Periods might start earlier or later than usual. Some women might skip months and then experience heavier periods when they do menstruate.
Symptoms Of Perimenopause:
These symptoms arise due to the ovaries producing less estrogen, leading the body to adjust to functioning with reduced levels of this hormone. The intensity and type of symptoms vary among women.
It’s essential to consult a doctor during perimenopause to rule out other potential causes for the symptoms. For instance, heavy or unexpected bleeding could indicate fibroids or uterine cancer, while night sweats and a racing heartbeat might be signs of a thyroid disorder.
Managing Perimenopausal Symptoms: Lifestyle changes can significantly help in alleviating perimenopausal symptoms. These include practicing yoga, engaging in regular exercise, meditation, and weight loss if necessary. Hormone therapy, vaginal estrogen treatments, and antidepressants can also be beneficial. It’s crucial to work with a gynecologist to develop a tailored treatment plan.
Discover our Quinoa and Roasted Vegetable Salad – a menopause-friendly dish packed with protein, vitamins, and antioxidants. Perfect for balancing blood sugar, boosting mood, and supporting heart health. Dive into a tasty, nutritious meal in just 35 minutes.
| Serving Size | Time | Difficulty |
|---|---|---|
| 2-3 | Prep Time: 10 minutes Cooking Time: 25 minutes Total Time: 35 minutes | Super Easy |
Remember that these are approximate values and can vary based on the specific sizes, preparation methods, and brands of ingredients used. For a detailed nutritional count, you’d need to use a specific nutrition calculator or software that takes into account the exact brands and quantities of each ingredient.

When we talk about menopause, the discussion often revolves around women – their experiences, challenges, and treatments. But how much do men know about this transition in their partners’ lives? A 2019 study published in the National Library of Medicine delved into the understanding and perceptions men have regarding menopause and its implications on their relationships.
To get a deeper insight into how men perceive menopause, an online survey1 was conducted. The questionnaire included 35 questions tailored to understand men’s attitudes and knowledge about this phase in a woman’s life.
Criteria for Participation: Men whose female partners, aged between 45-64 years, displayed at least one menopause-related symptom like hot flashes, sleeplessness, or mood swings. For context, the couples either shared a home or spent significant time together, at least a couple of times a week.
This study showcases that men are not just bystanders during their partner’s menopausal transition. They observe, they understand, and they even influence treatment decisions. However, there’s a need to amplify men’s knowledge about menopause and available treatment interventions. Providing more education on the topic can lead to better understanding, empathy, and support.
At the beginning of the video2, Dr. Sharon Parrish introduced a newly published survey on men’s perceptions and attitudes toward menopause. She emphasized the importance of understanding the male partner’s perspective, as they can offer valuable insights into the impact of menopausal symptoms both on the woman experiencing them and the man himself.
Dr. Parrish noted that past research has mostly focused on the woman’s perspective, leaving a gap in knowledge regarding the male viewpoint. There were some studies that looked into the male partners of menopausal women either individually or alongside their partners, but these were smaller and didn’t cover as much ground.
This recent study, named the MATE survey (Men’s Perceptions and Attitudes Toward Menopause), stood out. It was a comprehensive study targeting male partners of women undergoing menopause. Over 1,300 men were given a 35-question online survey, and around a third responded.
The primary aim of the survey was to gauge men’s awareness of their partner’s menopausal symptoms and to see if they played a role in influencing decisions about symptom management. If it was found that men were indeed influential in such decisions, then creating educational programs tailored for them could potentially benefit both partners by enhancing understanding of menopausal symptoms and treatment options.
The survey was wide-ranging in its approach. Men identified their partners’ menopausal symptoms and described how these symptoms affected them, their partners, and their relationship as a whole. The survey also asked about their communication and support strategies during this transitional period.
One significant finding was the majority of male respondents expressed comfort in discussing treatment options with their partners. Specifically, 65% of the respondents were open to such discussions, and a whopping 75% felt they could be influential in helping their partners make lifestyle changes or seek treatment for their menopausal symptoms.
Based on these findings, Dr. Parrish advocated for a shift in how we educate about menopausal symptom treatments. The results highlight that men in relationships with menopausal women are actively communicating with their partners about these symptoms. Their involvement and influence in discussions and decisions related to treatment can be pivotal.
Conclusively, Dr. Parrish emphasized that there exists an untapped opportunity. By educating men about menopause, they are better equipped to support their partners, offering more informed opinions on symptom management. This, in turn, could encourage more women to seek treatments, leading to better outcomes for menopausal women and their partners.
1Parish SJ, Faubion SS, Weinberg M, Bernick B, Mirkin S. The MATE survey: men’s perceptions and attitudes towards menopause and their role in partners’ menopausal transition. Menopause. 2019 Oct;26(10):1110-1116. doi: 10.1097/GME.0000000000001373. PMID: 31188286; PMCID: PMC6791510.
2The video above is published under Supplementary Materials, Supplemental Digital Content, menop-26-1110-s001.mov (39M) | GUID: 769B9ED7-81D6-42AD-95B7-1842B2A7D099
Copyright © 2019 The Author(s). Published by Wolters Kluwer Health, Inc. on behalf of The North American Menopause Society.
This is an open access article distributed under the terms of the Creative Commons Attribution-Non Commercial-No Derivatives License 4.0 (CCBY-NC-ND), where it is permissible to download and share the work provided it is properly cited. The work cannot be changed in any way or used commercially without permission from the journal. http://creativecommons.org/licenses/by-nc-nd/4.0
As with any significant change, it comes with its set of challenges. Physical, emotional, and psychological symptoms can be intense for some, while others may have a milder experience. Taking care of yourself during this transition can help you navigate it with more ease and resilience. Here are some self-care tips for thriving through menopause:
Menopause is a unique experience for every woman, and it’s essential to remember that there’s no one-size-fits-all approach. What works for one woman might not work for another. It’s crucial to listen to your body, communicate with healthcare professionals, and find what combination of self-care strategies works best for you.
As women transition from their reproductive years into menopause, their bodies undergo numerous changes that can have profound effects on various aspects of health, including menstrual cycles. One of the most noticeable changes during this phase, known as perimenopause, is the alteration in menstrual patterns. Understanding these changes can help women understand and better manage this critical phase of life with better confidence and awareness.
Perimenopause is the transitional phase that signals the onset of menopause. It typically begins in a woman’s 40s but can start earlier. One of the most significant hallmarks of this phase is the fluctuating estrogen levels produced by the ovaries. Estrogen, as we know, plays a pivotal role in regulating the menstrual cycle.
As a woman progresses through perimenopause, the ovaries’ production of estrogen diminishes. With this decrease, the regularity and pattern of menstrual cycles can become unpredictable. For instance, some months might witness the release of an egg – a process known as ovulation – while other months might not. The outcome is a menstrual cycle that’s less predictable than before.
As one nears menopause, there can be noticeable changes in the period’s duration and flow. Some women might experience shorter periods, while others could find their menstrual bleeding extending for more days than they were accustomed to. The interval between periods might lengthen or shorten. Furthermore, the volume of menstrual bleeding can vary, with some women reporting heavier bleeding and others experiencing lighter flows. It’s also not uncommon for women in perimenopause to skip periods altogether.
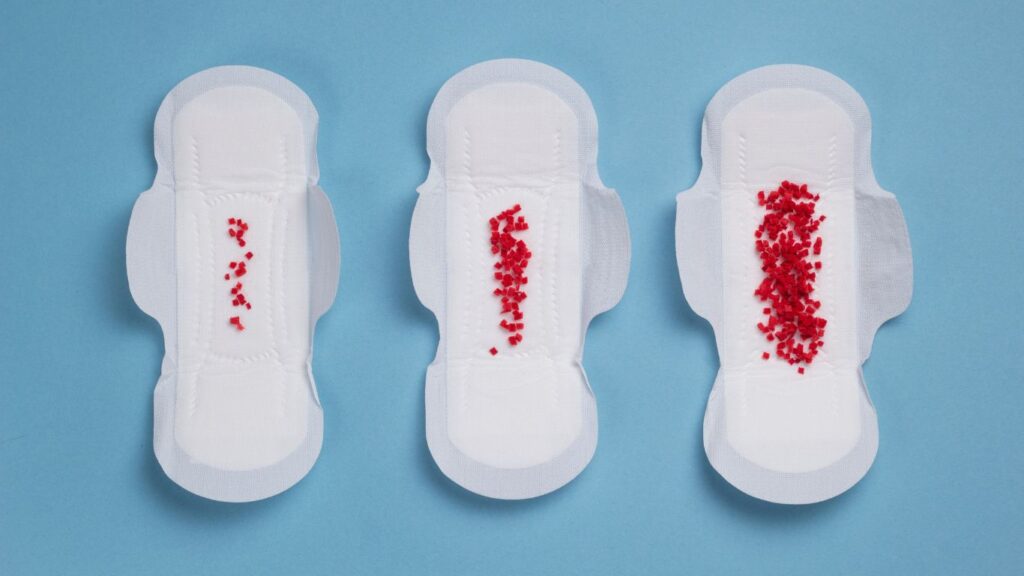
While irregularities become a norm during perimenopause, it’s essential to differentiate between expected variations and signs of potential health concerns. So, how does one ascertain if their bleeding is abnormal?
Perimenopause is an inevitable phase that every woman must traverse as she moves from her reproductive years into menopause. While it brings along many changes, particularly concerning menstrual patterns, knowledge and awareness remain the most potent tools in understanding this phase effectively. Recognizing what’s a part of the natural progression and what signals a potential health concern ensures that women remain proactive about their health, seeking timely intervention when needed. As always, maintaining an open channel of communication with a trusted gynecologist can make this journey smoother and more informed.

During perimenopause and menopause, hormone levels fluctuate and then decrease, which can result in a range of symptoms including hot flashes, night sweats, mood swings, and weight gain, among others. Some foods and drinks can exacerbate these symptoms. While every woman’s body is unique and may react differently, the following are commonly cited as potential “trigger” foods and beverages for menopausal symptoms:
Remember, the above are general guidelines and not all women will react to these foods in the same way. It’s essential to listen to one’s body and observe how it reacts after consuming certain foods. If a particular food seems to trigger symptoms, it may be beneficial to reduce or eliminate it and then see if symptoms improve.
In addition to being mindful of potential trigger foods, women going through perimenopause and menopause may also benefit from:
Always consult with a healthcare or nutrition professional when making significant changes to your diet, especially during a transitional phase like perimenopause or menopause.

Here’s a recipe for Salmon and Spinach Salad, which is rich in omega-3 fatty acids, antioxidants, and other nutrients that can be beneficial during menopause.
| Serving Size | Time | Difficulty |
|---|---|---|
| 2 | Prep Time: 10 minutes Cooking Time: 12-15 minutes Total Time: 22-25 minutes | Super Easy |
Benefits:
Enjoy your meal!

Please note that the values are approximate and can vary based on the specific sizes and brands of ingredients used. For an exact nutritional count, you’d need to use a specific nutrition calculator or software that takes into account the exact brands and quantities of each ingredient.
As women transition through various phases of life, personal growth and adaptation become paramount. Menopause and its preceding stage, perimenopause, bring about numerous changes—both physically and emotionally. However, this time also presents a unique opportunity for women to rediscover themselves and prioritize self-care. Let’s delve into ways to fully embrace this period of transformation.
Get to know your new self.
This transition isn’t just about hormonal shifts; it’s about embracing a new chapter. Dedicate time to self-reflection. Understand how your body and mind are changing. Acknowledging and accepting these changes can be empowering and pave the way for a positive outlook.
Find a new hobby.
Ever wanted to learn painting, dancing, or perhaps a new language? Now might be the perfect time. A new hobby can not only divert your mind from the challenges but also help you discover latent talents and passions.
Schedule regular “me time.”
Whether it’s a spa day, reading a book, or simply sitting in silence, carve out moments in your schedule that are exclusively for you. This time is essential for mental and emotional rejuvenation.
Know your limits.
With fluctuating energy levels, it’s crucial to understand and respect your boundaries. Don’t overexert yourself. Prioritize tasks and learn to say no when needed. Your well-being should always be at the forefront.
Focus on what you have, not what you don’t.
It’s natural to grieve the loss of one’s younger self or previous routines. However, shift the perspective. Celebrate the wisdom, resilience, and experiences you’ve gathered. Cultivate gratitude for the present moment.
Eat well and regularly to maintain stable blood sugar levels.
Diet plays a crucial role during this transition. Prioritize balanced meals that stabilize your blood sugar. Incorporate whole foods, reduce processed ones, and ensure you get essential nutrients to support your changing body.

Download a period-tracking app and keep a journal.
These tools can be invaluable. While the period tracker will help you note patterns and anticipate changes, a journal offers an emotional outlet. Jot down feelings, symptoms, or any significant occurrences. This record can be useful for both emotional processing and medical consultations.
Talk to someone about challenges you’re facing, especially if you think you may be depressed or anxious.
You’re not alone in this journey. Speak to friends, family, or professionals. Sharing your experiences can be cathartic and provide valuable insights. Mental well-being is paramount, and seeking support is a sign of strength, not weakness.
Takeaway
Embracing change can indeed be daunting, but remember that each phase of life comes with its unique beauty and challenges. Prioritize your well-being, indulge in ‘Me Time’, and view it as a beautiful opportunity to recharge. After all, every sunrise brings a new day, filled with possibilities. So, cherish the ‘Me Time’, for it equips you to face the world with renewed energy and grace.
Amid the increasing rise of female health champions and outspoken celebrities, the cloud of misconceptions and stigmas attached to menopause is finally lifting. Leading this charge is the stunning actress Naomi Watts. Her journey through menopause wasn’t smooth sailing, but she’s bravely opted to share it, emphasizing that it’s an inevitable phase for women.

At 36, just when Naomi was considering starting a family, she unexpectedly entered early menopause. This caught her off-guard, leading to feelings of isolation and panic. The actress candidly revealed her challenges, including fertility struggles, in a heart-to-heart with Drew Barrymore, even as she pampered her with a unique menopausal facial massage.
Now 54, Naomi is on a mission to enlighten and support women navigating this significant shift. She has initiated an online platform, “The Hot Spot”, for women to share and find solace in collective experiences amidst the tumultuous hormonal shifts.
Through her Instagram, Naomi disseminates crucial information. One video, for instance, elaborates on prevalent menopause symptoms like hot flashes, mood swings, weight fluctuations, and sleep disturbances.
Naomi aspires to educate women on what lies ahead, equipping them to handle the imminent physical and emotional evolutions more effectively. Always the optimist, Naomi emphasizes the silver linings, discussing the positives of menopause, like freedom from PMS and monthly cycles, in one uplifting video.
Her commitment extends beyond social media. Naomi has recently introduced her own brand dedicated to easing the menopausal journey. Yet, for Naomi, it’s not just about products—it’s about forging a community that understands and caters to women’s unique needs during this phase. Reflecting on her own confusion when menopause hit, she aims to provide clarity and guidance to others.
Ultimately, Naomi’s vision is clear: Normalize menopause dialogues and eradicate the associated stigmas. She’s confident that women, when informed, can be the strongest advocates for menopausal health.
What’s your menopause story? Had a support system to lean on? Share your experiences below.
While the hormonal shifts of the menopause stage can be challenging, understanding their impact on our skin is pivotal. In this blog, we’ll explore the relationship between skincare and menopause, shedding light on essential practices and products that can help maintain skin vitality. No need for overly technical jargon – just clear insights to support you during this unique chapter of life. Let’s dive into the world of menopausal skincare together.
During the menopause stage, the body produces fewer estrogens, which can lead to:
What’s happening?
Estrogen, a primary female sex hormone, plays a key role in maintaining skin moisture and elasticity. As women approach and experience menopause, there’s a noticeable drop in estrogen levels.
Impact on the skin:
This hormonal shift directly affects the skin’s ability to produce oil (sebum) and the protein collagen. Sebum acts as a natural moisturizer, preventing skin from drying out. Meanwhile, collagen is responsible for giving skin its firmness and youthful bounce. As production of both sebum and collagen decrease, the skin becomes drier and loses its plump, firm appearance, making it more susceptible to external stressors and dehydration.
What’s happening?
Hot flashes are a common symptom of menopause, resulting from the body’s reaction to decreasing estrogen levels. This reaction often leads to a sudden and temporary surge in body temperature.
Impact on the skin:
During a hot flash, blood vessels close to the skin’s surface expand to help cool down the body, causing a noticeable flush or redness, particularly on the face and neck. Though temporary, frequent hot flashes can lead to persistent redness and irritation over time.
What’s happening?
The protective barrier of our skin, often termed as the lipid barrier, weakens with a reduction in estrogen levels.
Impact on the skin:
A compromised barrier means that the skin is less effective in keeping out potential irritants, be it from skincare products or environmental pollutants. Consequently, the skin becomes more reactive, leading to increased sensitivity, irritation, and even the potential for allergic reactions.
What’s happening?
Beyond collagen, estrogen also aids in the production of elastin, another protein that helps skin bounce back after being stretched.
Impact on the skin:
With reduced estrogen levels during menopause, there’s a decline in both collagen and elastin. This causes the skin to become thinner, more fragile, and less resilient to physical and environmental stressors. The thinning skin is also more prone to bruising and damage.
What’s happening?
The combined effect of decreased collagen production, environmental factors, and natural aging processes accentuate the appearance of wrinkles.
Impact on the skin:
Collagen provides structure and volume, and as its production decreases, the skin loses its firmness. This, combined with years of sun exposure, environmental pollutants, and other external damage, deepens existing wrinkles and promotes the formation of new ones. Regular sun protection and skincare tailored to mature skin can help in mitigating these effects.
Stay Hydrated Inside and Out: Drinking plenty of water helps, but also invest in a good moisturizer. Look for ingredients like hyaluronic acid, ceramides, and glycerin which lock in moisture.
Gentle Cleansing: Opt for a mild, hydrating cleanser. This will prevent stripping your skin of its natural oils, which are already reduced during menopause.
Incorporate Sun Protection: UV rays contribute significantly to premature aging. Use a broad-spectrum sunscreen daily, even if you’re indoors.
Retinoids are Your Friend: Consider using products with retinoids. They help in boosting collagen production, which can combat wrinkles and improve skin texture.
Antioxidants for the Win: Serums containing Vitamin C, E, and ferulic acid can help combat free radical damage, promoting radiant skin.
Don’t Forget Your Eyes and Neck: These areas can show signs of aging more rapidly during menopause. Invest in a good eye cream and neck cream to address specific concerns.
Gentle Exfoliation: Remove dead skin cells and rejuvenate the skin with mild exfoliants. This encourages cell turnover and boosts radiance.
Hormone Replacement Therapy (HRT): Consult your healthcare provider about HRT. It can alleviate some menopausal symptoms and may have positive effects on the skin.
Balanced Diet: Ensure your diet is rich in antioxidants, Omega-3 fatty acids, and vitamins. Foods like fish, nuts, berries, and green leafy vegetables can promote healthier skin.
Regular Exercise: Physical activity can boost circulation, giving your face a healthy glow and aiding in skin cell renewal.
Manage Stress: Stress can exacerbate skin issues. Consider relaxation techniques like meditation, yoga, or simply taking time for yourself.
Avoid Smoking and Limit Alcohol: Both can accelerate skin aging and exacerbate dryness.
There are a plethora of treatments and professional skincare services tailored for menopausal skin, from lasers to facials. Consult a dermatologist to understand which might be suitable for you.
Remember, ladies, menopause is a natural phase of life. With the right care and a dash of self-love, you can navigate through it with grace, confidence, and glowing skin. Embrace this chapter and let your inner beauty shine through! 💫
Many believe that hair loss or pattern baldness is a challenge solely faced by men. In reality, various factors, including the hormonal fluctuations associated with stages such as perimenopause and menopause, can trigger hair loss in women too. Aside from these stages of life, other underlying medical conditions, certain medications, and even high-stress episodes can contribute to hair thinning or loss. However, the most common culprit remains female pattern baldness, a genetically and hormonally driven condition that progressively affects a substantial number of women.
This hair loss often becomes noticeable during perimenopause and menopause, when hormonal changes are at their peak. The condition is primarily marked by a slow, steady thinning of hair, predominantly on the crown of the scalp.
Understanding Thinning Hair
Thinning hair manifests as a reduced density of hair predominantly on the crown of the scalp. Women often first become aware of this condition when they notice a widening of their hair parting or if their hair begins to feel more delicate and wispy. Over time, this reduction in hair density continues, making the scalp more visible. In severe cases, the crown may even exhibit a complete absence of hair, leaving a noticeable bald spot.
Taking Action
When dealing with hair loss, time is of paramount importance. Many hair disorders are time-sensitive, meaning the sooner you identify and address the issue, the better your chances of mitigating the impact. Therefore, if you begin to observe signs of hair loss, it’s advisable to promptly consult a hair specialist, such as a dermatologist.
Some Practical Advice
It’s crucial to treat your hair with care and gentleness. Reducing the frequency of washing your hair can help maintain its natural oils and strength. Additionally, avoid hairstyles that pull on the roots, like tight braids, or wearing constrictive headgear. Be careful about the products you apply on your hair, steering clear of those containing harsh chemicals that could potentially aggravate hair loss.
In an article on the American Academy of Dermatology Association (AADA) website, it’s highlighted that dermatologists often employ multiple hair-loss treatments concurrently to achieve the best outcomes for women. For FPHL, various treatment options are listed. Here are some of them:
As reported by the Mayo Clinic News Network, understanding the causes, recognizing the signs, and taking timely action can be the key to managing hair loss effectively. With a bit of care and attention, you can protect your hair’s health and vitality.
For many, menopause can feel like an intricate maze of physical and emotional changes. One navigational challenge that demands attention is the precarious decline in bone health. Research, unsettling as it might be, reveals a daunting acceleration of bone loss during menopause, with osteoporosis becoming a potential unwanted companion. In fact, a concerning 20% of bone loss can manifest during these pivotal stages, recent data from the International Osteoporosis Foundation highlights that 1 in 3 women (and 1 in 5 men) over 50 will endure osteoporotic fractures during their lives. Essentially, one fracture often signals the onset of more.
The implications? One in three postmenopausal women will eventually confront osteoporosis. More alarming is the prospect of fractures, which invariably lead to pain, decreased mobility, and a discernible dip in quality of life. Moreover, fractures carry with them a more ominous potential: a notable increase in mortality.
This isn’t a narrative of inevitable decline. On the contrary, data suggests that with timely intervention, older women can respond remarkably well to osteoporosis treatments. The objective becomes clear: strategically mitigate fractures and foster sustained bone health.
Diving deeper into the mechanics, osteoporosis, characterized by its literal translation “porous bones”, is chiefly propelled by menopause. Hormonal fluctuations, especially in estrogen levels, are intrinsic to the menopausal journey. Estrogen plays a pivotal role in curbing bone degeneration. As menopause ensues, and estrogen levels see a marked decrease, bone loss correspondingly intensifies.
Further down the hormonal spectrum is estradiol, a specific estrogen variant. As women transition through menopause, estradiol production wanes, often culminating in halted menstrual cycles. This hormonal shift can usher in a suite of familiar menopausal symptoms: mood fluctuations, vaginal dryness, hot flashes, and night sweats. In the long arc, diminished estradiol levels lay the groundwork for osteoporosis.
Finally, no discourse on bone health is complete without acknowledging the linchpins of bone vitality: Vitamin D and calcium. Vitamin D operates as the crucial mediator, facilitating calcium absorption — the foundational element for robust bones. A deficit in Vitamin D renders even a calcium-rich diet ineffectual, underscoring the duo’s indispensable role in bone fortification.
The following are some of the effective strategies to help prevent or slow down this process:
Maintaining good bone health involves not only incorporating beneficial foods into your diet but also limiting or avoiding those that can negatively impact bone density and strength. Here are some foods and drinks that may negatively affect bone health when consumed in excess:
While some of these foods have health benefits and are valuable in a balanced diet, it’s essential to consume them in moderation and be aware of their potential impact on bone health. Always balance your diet with a variety of nutrient-dense foods, and consult with a healthcare professional about specific dietary concerns.
Have you heard discussions about memory and menopause? Consider this: approximately 14 million individuals in the US may suffer from Alzheimer’s by 2050, with a significant majority being women. This is projected to cost the US around $2 trillion. Why the emphasis on women? Menopause often correlates with memory issues. Furthermore, women play a critical role in our global economy and frequently care for family members without monetary compensation. Therefore, prioritizing memory health during and after menopause is not merely a personal concern; it has broader implications for families, society, and the economy.
Rethinking Memory Decline: It’s Not Just for Your Golden Years
It’s a common assumption: As we get older, especially when we hit our 70s, we should expect some memory slip-ups. That’s just the way aging works, right? Well, not so fast. While it’s true that age can influence cognitive functions, we might be doing ourselves a disservice by waiting for the later years to start addressing it.
Memory decline, often viewed as an inevitable companion of our golden years, is indeed a part of the aging spectrum. However, it doesn’t just suddenly show up when we celebrate certain milestone birthdays. The groundwork for how our brains will function in later life is laid much earlier.
Take the middle years of our life, for example. These years, spanning from our 40s to 60s, are more crucial to our cognitive future than many of us realize. It’s a period marked by significant hormonal changes, lifestyle adjustments, and varying stressors – all of which can influence brain health.
But here’s the kicker: it isn’t solely about the looming threat of diseases like Alzheimer’s or other forms of dementia. It’s about the subtle, yet profound, shifts in our cognitive functions that can reshape how we interact with the world, make decisions, and even how we perceive emotions and experiences.
By tuning into these changes and understanding them, we can proactively address potential challenges and harness the strengths that come with age. Instead of bracing for decline, we can equip ourselves with knowledge and strategies that amplify our brain’s resilience.
In a nutshell, our approach to brain health and memory shouldn’t be a reactive game, played when we detect the first signs of slip-ups. It should be a proactive journey, starting in midlife, focused on nourishing and optimizing our most vital organ for the adventures ahead.
The Menopausal Brain Shift
Menopause isn’t just hot flashes and mood swings. It’s a phase where women’s bodies undergo reproductive aging. With the gradual depletion of hormones like estradiol (a type of estrogen vital for our brains), women might notice shifts in their memory game. The good news? This isn’t a universal experience. While some women breeze through, others might be wrestling with forgetfulness or “brain fog.”
At the heart of menopause is the shift in reproductive aging. The ovaries start to retire from their hormone production role, leading to a decrease in hormones, notably estradiol. Estradiol is no ordinary hormone; it’s a type of estrogen that holds a VIP pass to our brain functions, particularly memory.
Now, here’s where things get intriguing. As these hormonal levels wane, some women might experience what feels like a memory roller coaster. They may find themselves pausing to recall a familiar name or momentarily misplacing everyday items more often. Terms like “brain fog” aren’t just catchy phrases; they resonate with the lived experiences of many women during this transitional phase.
Yet, it’s crucial to emphasize the spectrum of experiences. Menopause isn’t a one-size-fits-all journey. Some women continue to navigate their daily lives with the cognitive agility of their younger selves, while others might feel like they’re treading through mental molasses.
But what’s behind these cognitive quirks? The past 15 years of research have been nothing short of revelatory. Menopause doesn’t just initiate hormonal shifts; it reshapes the very architecture and dynamics of our brain. This period can influence how our brain cells interact, the efficiency of their communication highways, and even determine how long these cells thrive.
Furthermore, as estrogen levels decrease and with it the brain’s glucose supply, our brain showcases its adaptability. Much like a seasoned traveler finding alternative routes when a road is blocked, the brain begins to tap into different metabolic pathways, seeking other sources of fuel to keep its functions running smoothly.
The Additional Risks
But there’s more to the story. Toss in chronic conditions like diabetes and hypertension, and you’ve got a more intricate game at hand. These health issues complicate the narrative. Our brain and body share a profound, intertwined relationship – how our body produces energy, how our blood vessels function, it all ties back to our cognitive health. For women battling these conditions, understanding this intricate dance between brain-body functions becomes even more vital. It’s like putting together a puzzle where every piece impacts the bigger picture.
To HR or Not to HR: The Hormone Dilemma
Hormone Replacement (HR) has become quite the buzzword. But, as with most health decisions, context is king. Starting HR isn’t like flipping a switch. It’s about timing, and believe it or not, that clock can tick differently for each woman. Dive in too early or too late, and you might be met with unforeseen challenges. Sure, HR might seem like a godsend for some, especially those who’ve faced an early ovary removal. But it’s no panacea. For every success story, there are tales of mismatched expectations. And if you find yourself in the ‘HR isn’t for me’ camp, fear not. The realm of medical research is vast and ever-evolving, with scientists tirelessly exploring avenues beyond HR.
Your Brain Health Playbook
Want to give your brain a fighting chance? Imagine crafting a care package for your brain. What would you put in it? At the core, three elements stand out:
When we think of hitting the gym, visions of toned muscles and cardiovascular endurance often dance in our heads. But here’s a twist for you: imagine your brain donning sporty gym shorts and lifting weights. Sounds funny, right? Yet, in essence, that’s what’s happening. Each time you engage in physical activity, from a leisurely stroll in the park to a high-intensity spin class, your brain benefits. Every heartbeat pumps more oxygen-rich blood to the brain, promoting the growth of new neurons and connections. In essence, every drop of sweat isn’t just helping you shed calories, but it’s ensuring your brain stays nimble and robust. It’s like paying dues for a gym, where the currency is effort and the reward is cognitive health.
Ever felt the satisfaction of completing a challenging crossword puzzle or finally mastering a difficult chapter in a book? That’s not just a pat on the back for persistence. It’s your brain flexing its muscles after an intense workout session. Engaging in cognitive challenges, whether it’s solving a mathematical problem, diving into a gripping novel, or picking up a new instrument, stimulates different regions of the brain. It’s like circuit training, where each new challenge targets a unique ‘muscle group’ in the brain, strengthening cognitive pathways and enhancing mental agility. So the next time you challenge yourself to a game of chess or decide to learn a new language, remember: you’re not just passing the time; you’re sculpting a fitter, sharper mind.
Picture a dance floor, vibrant with energy, alive with movement, each dancer bringing a unique rhythm and style. That’s the scene inside our brain during social interactions. When we engage in conversations, share a laugh, or partake in hearty debates, our brain lights up in a dynamic dance of neural activity. Different regions synchronize and communicate, processing emotions, recalling memories, and formulating responses. It’s not just about staying socially active; it’s about the richness of human connection. These interactions stimulate our emotional and cognitive processes, ensuring our brain remains engaged and active. In essence, every interaction is a step, a move, a groove on the vast dance floor of our minds, keeping it vibrant and youthful.
Add to that a sprinkle of healthy dietary habits and the magic potion of adequate sleep, and you’re setting yourself up for success. These aren’t just tips; they’re lifelines, especially for those at a higher risk of cognitive decline.
To sum it up, understanding menopause’s impact on brain health isn’t just a “nice-to-know.” It’s a must. And while more research is in the pipeline, there’s no time like the present to be proactive. Ladies, the power to shape our cognitive future is, in many ways, in our hands.
Explore energy-boosting foods that can help combat the fatigue often associated with menopause, ensuring vitality and well-being.
During menopause, there are a number of changes that occur in a woman’s body, including changes in hormone levels, body composition, and energy expenditure.
One of the most significant changes that occurs at menopause is a decline in estrogen levels. Estrogen is a hormone that plays a number of important roles in the body, including regulating metabolism and fat storage. When estrogen levels decline, it can lead to changes in body composition, including a decrease in fat-free mass (muscle and bone tissue) and an increase in fat mass.
Another change that occurs at menopause is an increase in follicle-stimulating hormone (FSH) levels. FSH is a hormone that helps to regulate the production of eggs in the ovaries. When estrogen levels decline, FSH levels rise. This can also lead to changes in metabolism and fat storage, which can contribute to weight gain.
In addition to changes in hormone levels, menopause can also lead to changes in energy expenditure and spontaneous activity. Energy expenditure is the amount of energy that the body uses to maintain its basic functions. Spontaneous activity is the amount of activity that is done without any conscious effort, such as fidgeting or walking around. Both energy expenditure and spontaneous activity tend to decrease after menopause, which can contribute to weight gain.
A study published by Journal of Mid-life Health1 suggests that women gain an average of 1-2 pounds per year after menopause. Other studies have found that women gain as much as 10-15 pounds during this time. Below are some of the highlights from the study:
What Causes Menopause-Related Weight Gain?
There are a number of factors that can contribute to menopause-related weight gain. One factor is the decline in estrogen levels. Estrogen is a hormone that helps to regulate metabolism and fat storage. When estrogen levels decline, it can lead to changes in body composition, including a decrease in fat-free mass (muscle and bone tissue) and an increase in fat mass.
Another factor that can contribute to menopause-related weight gain is the increase in follicle-stimulating hormone (FSH) levels. FSH is a hormone that helps to regulate the production of eggs in the ovaries. When estrogen levels decline, FSH levels rise. This can lead to changes in metabolism and fat storage, which can contribute to weight gain.
How Can I Prevent Menopause-Related Weight Gain?
There are a number of things that you can do to prevent menopause-related weight gain. These include:
If you are concerned about menopause-related weight gain, talk to your doctor. They can help you to develop a personalized plan to help you lose weight and keep it off.
What Else Should I Know?
In addition to the factors mentioned above, there are a few other things that you should know about menopause-related weight gain.
Here’s something to think about: women going through menopause who are overweight tend to have a tougher time with symptoms. Losing weight can boost their mood, self-worth, and overall well-being. And when it comes to intimacy, some studies suggest that obesity can affect satisfaction and function. It’s also worth noting that how we feel about our bodies can deeply impact our mental health. If you are concerned about menopause-related weight gain, talk to your doctor. They can help you to develop a personalized plan to help you lose weight and keep it off.
1 Fenton, Anna. Weight, Shape, and Body Composition Changes at Menopause. Journal of Mid-life Health 12(3):p 187-192, Jul–Sep 2021. | DOI: 10.4103/jmh.jmh_123_21
Hey there, lovely readers! Let’s dive into a topic that’s been on the minds of many but isn’t always discussed openly: mood swings during menopause. If you’ve ever wondered why your emotions seem to be on a wild ride during this phase of life, you’re not alone. Let’s break it down, shall we?
First things first, what’s causing these mood swings? Menopause is a natural part of aging, marking the end of a woman’s reproductive years. As the ovaries produce fewer hormones, namely estrogen and progesterone, it can lead to a range of symptoms, including those unpredictable mood swings.
A recent study from Harvard Medical School explains that these hormonal changes can influence neurotransmitters in the brain, which are closely linked to mood. So, it’s not just “all in your head” – there’s real science behind it!
While hormones play a significant role, they’re not the only culprits. Sleep disturbances, which are common during menopause, can also contribute to mood swings. A lack of sleep can make anyone irritable, right? Plus, life changes, like kids leaving home or facing one’s own aging process, can add emotional stress.
Now, while I’m no doctor, there are some general tips that many find helpful during this transition:
The Science Behind It:
Physical activity has long been associated with improved mental well-being. When you exercise, your body releases chemicals called endorphins. Often referred to as the body’s “natural painkillers,” endorphins promote a sense of well-being and can temporarily relieve pain.
Finding Your Groove:
The beauty of exercise is that it doesn’t have to be a structured gym session. It’s all about movement. A brisk walk in the park, a rejuvenating yoga session, or even dancing to your favorite tunes in your living room can get your heart rate up and those endorphins flowing. The key is consistency. Find an activity you genuinely enjoy, making it easier to incorporate into your daily routine.
The Power of Connection:
Humans are inherently social beings. Sharing experiences, especially challenges, can create a sense of belonging and understanding. Talking about what you’re going through can provide relief and perspective.
Finding Your Tribe:
Consider joining a menopause support group where you can connect with others going through similar experiences. If groups aren’t your thing, even confiding in a close friend or family member can make a world of difference. Remember, you’re not alone in this journey, and there’s strength in numbers.
The Science Behind It:
Mindfulness and meditation have been shown to reduce stress, improve focus, and promote emotional health. These practices encourage you to stay present, acknowledging your feelings without judgment.
Incorporating Mindfulness:
Start with deep breathing exercises, focusing on each inhale and exhale. This simple act can center your mind. Meditation, even if for just a few minutes a day, can create a sense of calm. Journaling, on the other hand, offers a space to express and process your emotions, providing clarity and perspective.
When to Seek Help:
While it’s natural to have ups and downs, if you find that mood swings are significantly affecting your daily life, it might be time to seek professional guidance.
The Role of Therapists and Counselors:
These professionals are trained to provide coping strategies tailored to your unique situation. They offer a safe space to discuss your feelings, fears, and concerns, helping you navigate the complexities of menopause with understanding and tools to manage the emotional roller coaster.
Menopause is a journey, and like all journeys, it comes with its challenges. But with understanding, support, and a few strategies up your sleeve, you can navigate this phase with grace and resilience.
Remember, every woman’s experience is unique. So, be kind to yourself, seek support when needed, and know that you’re not alone on this roller coaster ride.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice or treatment. Always consult with a healthcare provider about any health concerns.
We all know how important a good night’s sleep is for our overall well-being, especially during this transitional phase. Hormonal fluctuations, night sweats, and other symptoms can wreak havoc on our sleep quality. In this comprehensive guide, we will explore sleep hygiene practices tailored specifically for menopausal women. From creating a sleep-friendly bedroom environment to implementing relaxation techniques, let’s dive into some friendly and practical tips to optimize your sleep hygiene and enjoy those restful nights you deserve!
Creating a Sleep-Friendly Bedroom Environment
Your bedroom plays a crucial role in promoting quality sleep. Here are some tips to create a sleep-friendly environment during menopause:
Bedtime Routines and Rituals
Establishing a consistent bedtime routine signals to your body that it’s time to wind down and prepare for sleep. Here are some tips to optimize your bedtime routine during menopause:
Dietary Considerations for Better Sleep
What you eat and drink can impact your sleep quality. Consider the following dietary considerations during menopause:
Exercise for Restful Nights
Regular physical activity has been shown to improve sleep quality. Consider the following exercise tips for better sleep during menopause:
Stress Management Techniques
Managing stress is vital for better sleep during menopause. Here are some stress management techniques to incorporate into your daily routine:
Remember that every woman’s experience with menopause is unique. Be patient with yourself and open to trying different strategies until you find what works best for you. These tips and evidence-based recommendations are here to guide you, but ultimately, you’re the expert on your own body. Embrace this journey with a sprinkle of self-love, and prioritize your sleep to wake up refreshed and ready to conquer each day with a renewed sense of energy.
In the quiet hours of the night, many women find themselves jolted awake, sheets drenched and a heat wave coursing through their bodies. This isn’t the aftermath of a forgotten thermostat setting or a summer night’s humidity. It’s a more personal kind of heat, one that’s intimately tied to a natural phase of life: menopause. Night sweats, one of the hallmark symptoms of menopause, can be both baffling and frustrating. Let’s delve into this nocturnal nuisance and explore ways to find relief.
Menopause, often dubbed the “change of life,” is a significant milestone in a woman’s life, marking the end of her reproductive years. As the ovaries reduce their production of estrogen and progesterone, a cascade of physiological changes ensues. One of the most notable? The infamous hot flashes, which don’t discriminate between day and night.
Night sweats are essentially hot flashes that occur during sleep. The sudden drop in estrogen confuses the hypothalamus—the brain’s thermostat. Mistakenly believing the body is overheating, it triggers a rapid cooling process: dilated blood vessels, increased heart rate, and, of course, sweating.
When the serenity of sleep is repeatedly interrupted by night sweats, the consequences extend far beyond the immediate discomfort of damp sheets and pajamas. These nocturnal disruptions, often dismissed as mere inconveniences, can have profound implications for one’s overall well-being. Chronic sleep disruption can lead to a host of issues:
Cognitive Impact: The Brain’s Cry for Restful Sleep
Sleep isn’t just a passive state of rest; it’s an active process during which the brain undergoes essential maintenance. One of its primary roles is in memory consolidation, where the brain processes and stores new information from the day.
When night sweats disrupt this process, the aftermath isn’t just a groggy morning. Over time, these interruptions can manifest as:
Emotional Toll: The Delicate Balance of Mood and Sleep
Sleep and emotional well-being are deeply intertwined. A restful night acts as an emotional reset, allowing individuals to approach a new day with a balanced mindset.
However, when sleep is persistently disrupted:
Physical Health: The Silent and Cumulative Effects of Sleep Deprivation
The body uses sleep as a time for repair and rejuvenation. When this process is interrupted:
While night sweats might seem like an inevitable part of menopause, there are strategies to mitigate their impact:
Night sweats, while a common symptom of menopause, don’t have to define this phase of life. With informed choices and proactive measures, it’s entirely possible to navigate this midnight heat wave and find cooler, more restful nights ahead. As with any health concern, it’s crucial to consult with a healthcare provider to tailor a strategy that’s right for you.